Peripheral immune-inducer dendritic cells drive early-life allergic inflammation
TL;DR
Early-life allergen exposure triggers a unique immune response through peripheral immune-inducer dendritic cells (pii-DCs) in the skin, leading to type 17 inflammation. This process is enabled by immature neuroendocrine development and low glucocorticoid levels, shaping age-dependent allergic responses.
Key Takeaways
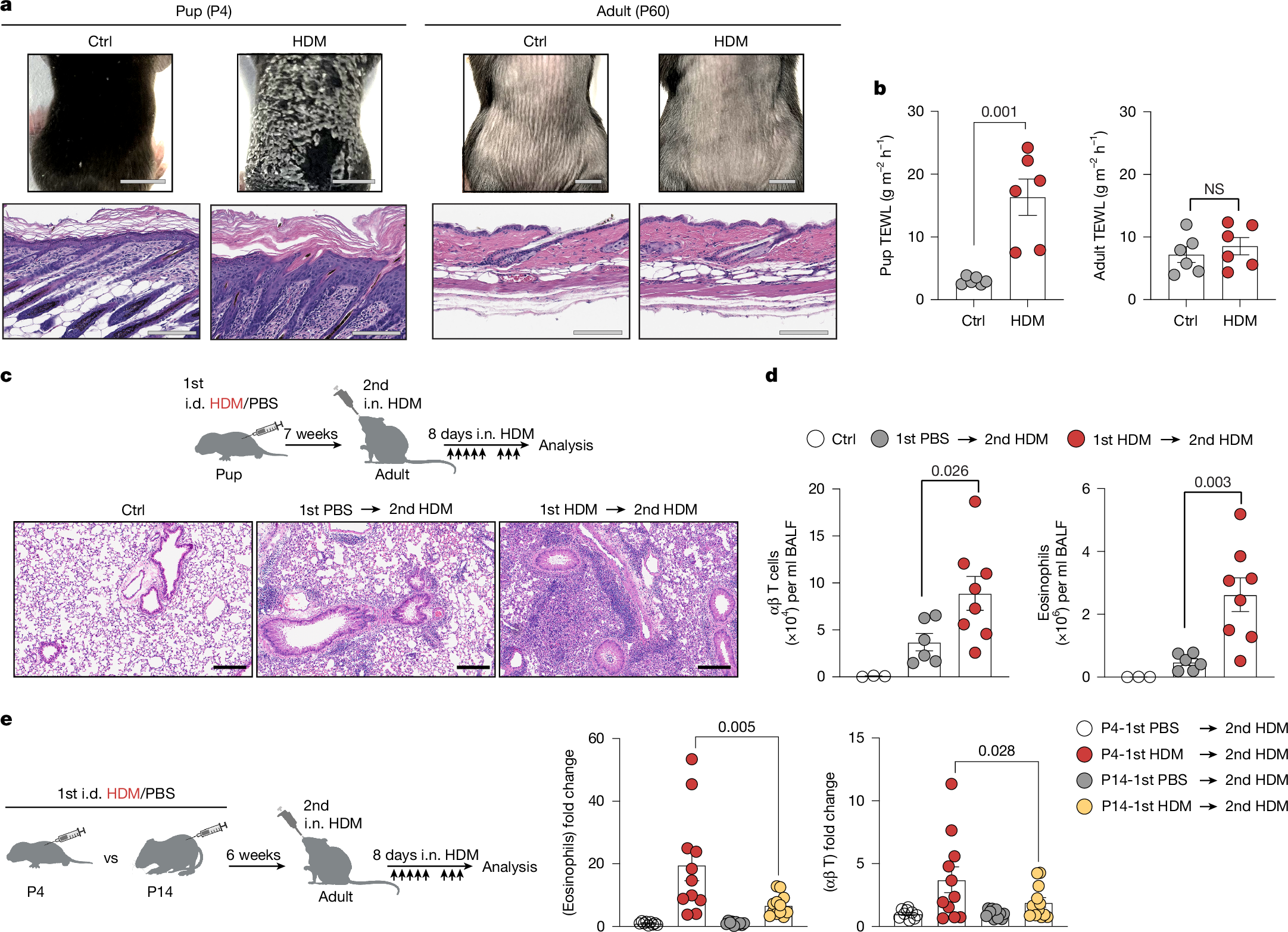
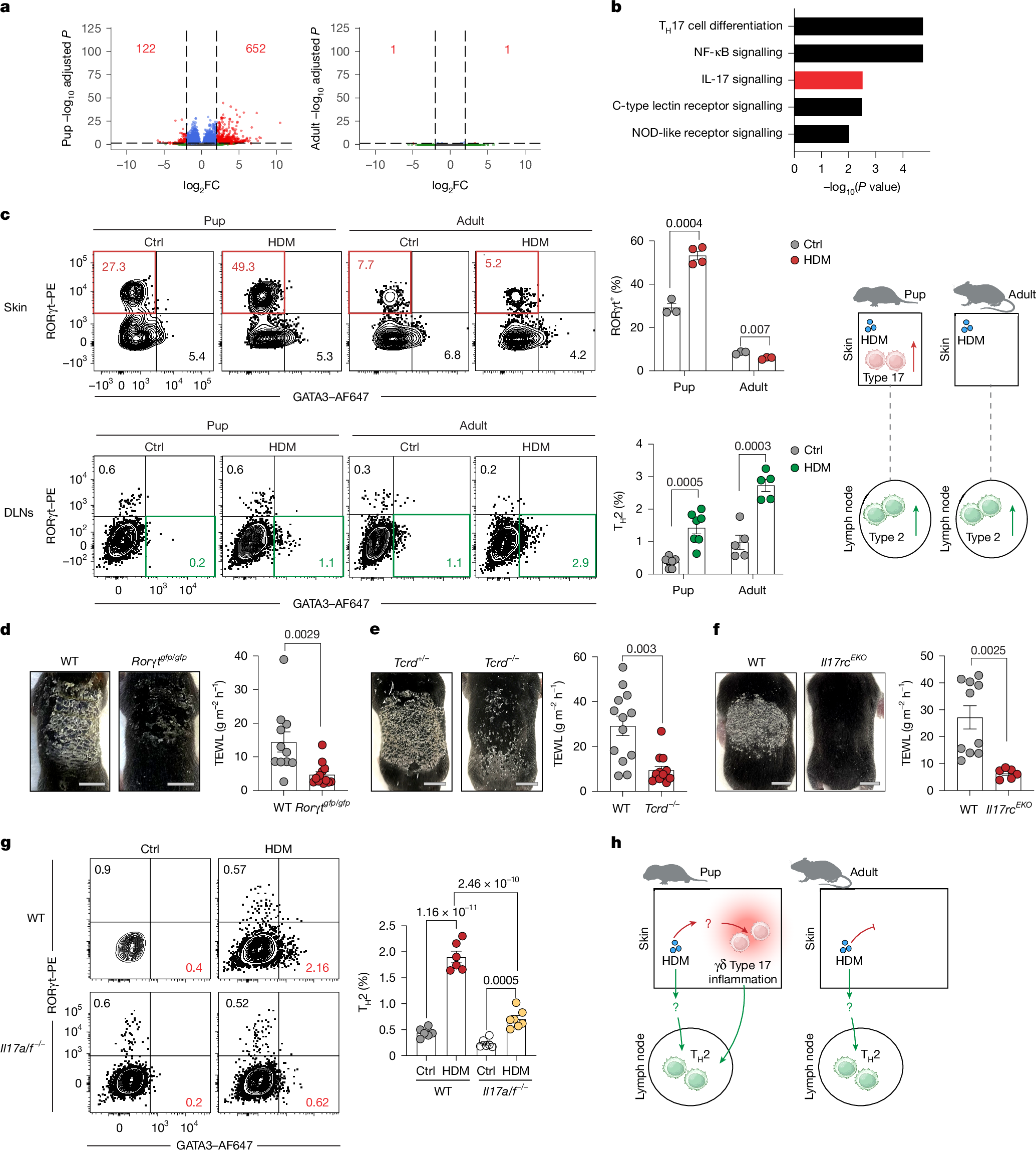
- •Early-life allergen exposure triggers simultaneous type 17 skin inflammation and T helper 2 sensitization in lymph nodes.
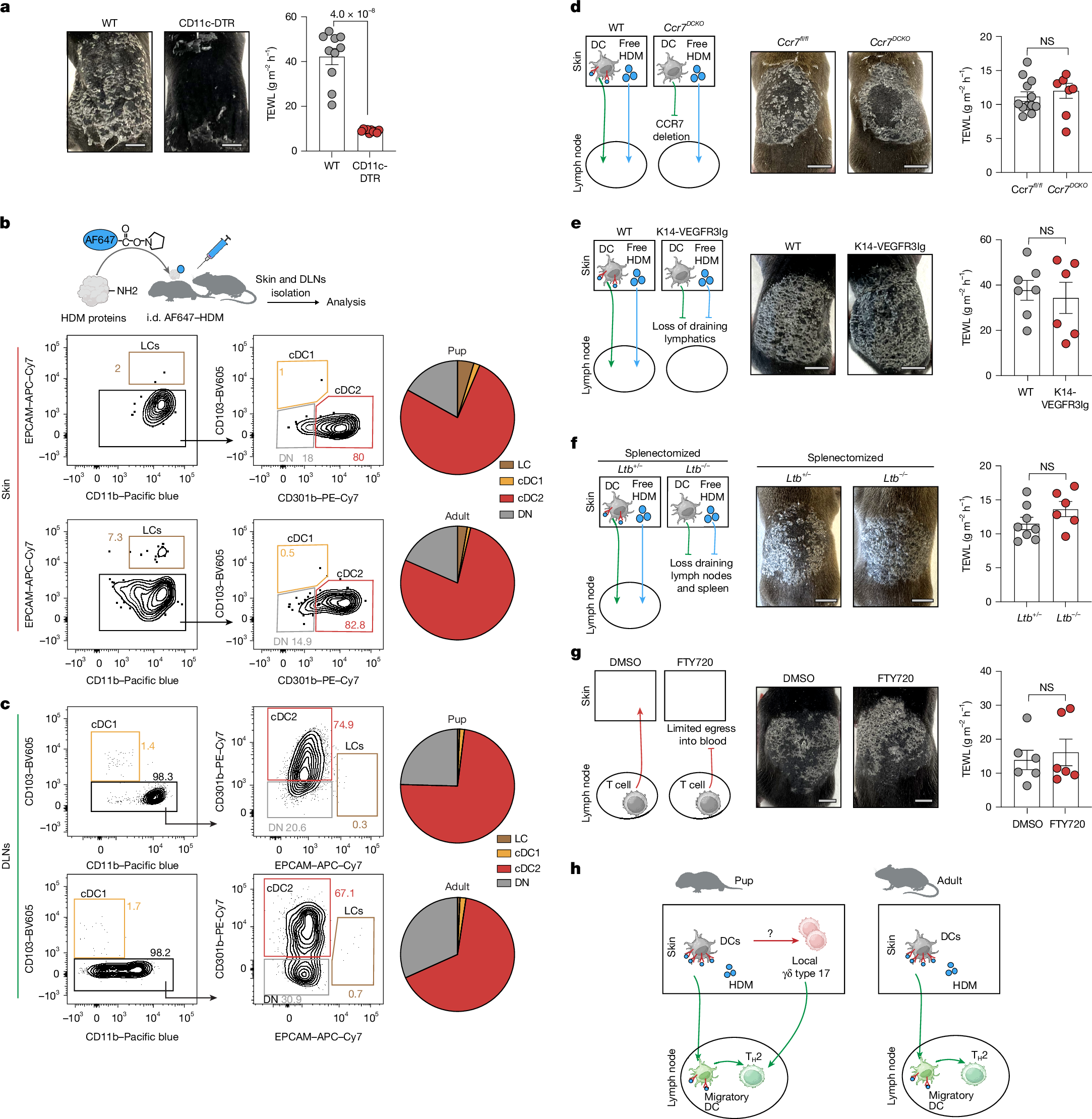
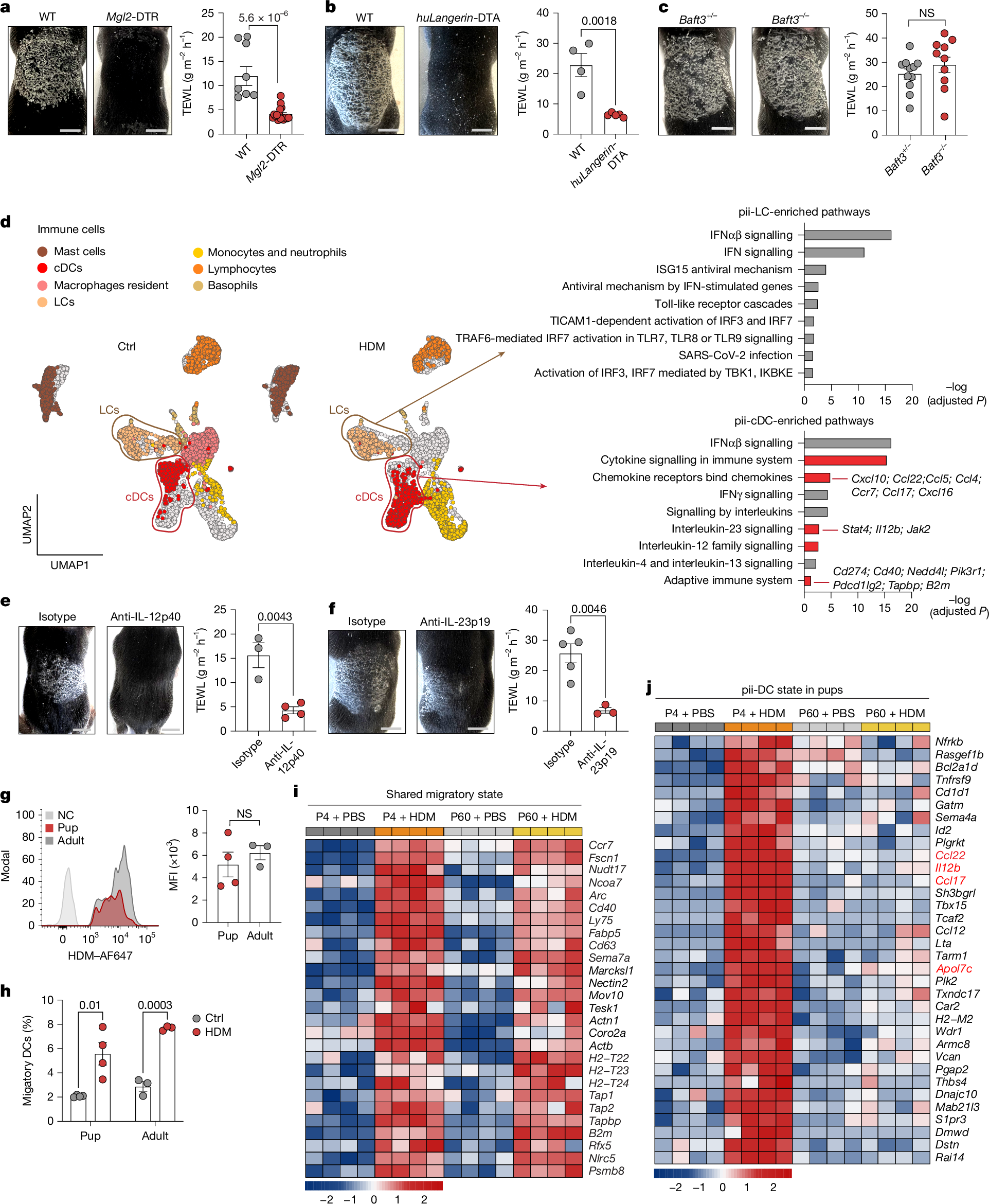
- •Peripheral immune-inducer dendritic cells (pii-DCs) activate type 17 immunity directly in the skin without lymph node migration.
- •The pii-DC state is enabled by immature hypothalamic-pituitary-adrenal axis development and low systemic glucocorticoids in early life.
- •This developmental checkpoint shapes age-dependent allergic responses and primes exaggerated lung inflammation upon secondary exposure.
Tags
Abstract
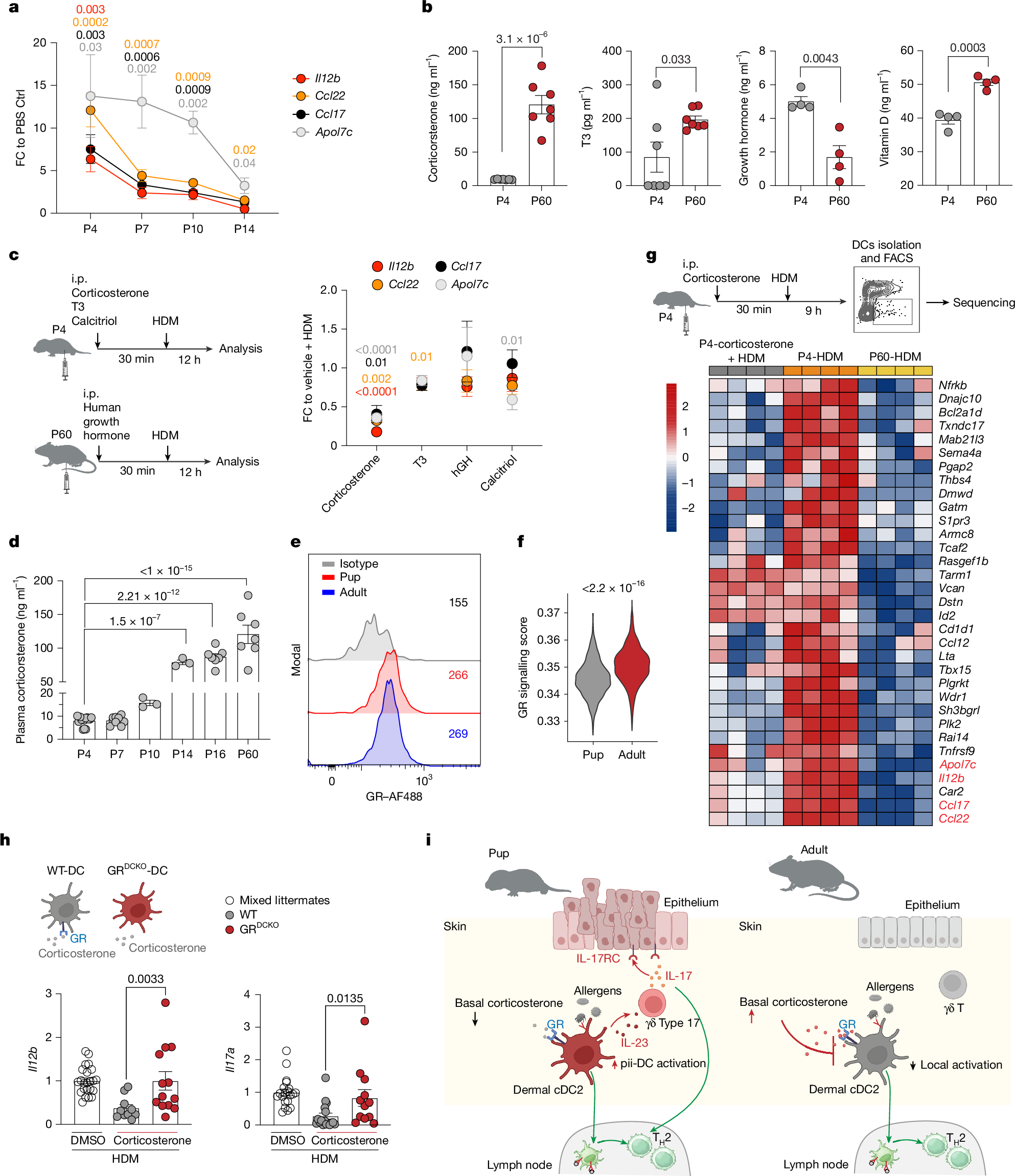
Atopic diseases associated with allergens, as well as allergic diseases, frequently arise early in life; however, the age-dependent mechanisms governing immune responses to allergens remain poorly understood1. Here we find that in early life, exposure to common allergens triggers a distinct bifurcated immune response, simultaneously triggering type 17 inflammation in the skin and initiating canonical T helper 2 sensitization in the lymph nodes. This early-life γδ type 17-mediated dermatitis primes the exaggerated allergic lung inflammation upon secondary allergen exposure. Mechanistically, we find dendritic cell (DC)-mediated type 17 activation directly in the skin without requiring migration to lymph nodes; we term this state ‘peripheral immune inducer’ (pii) DC. CD301b+ conventional type 2 DCs acquire allergen, adopt the pii-DC state, produce IL-23 and activate local γδ type 17 cells independently of lymph-node engagement. The pii-DC state is enabled by the immature hypothalamic–pituitary–adrenal axis and physiologically low systemic glucocorticoids characteristic of early life2,3; DC-specific deletion of the glucocorticoid receptor recapitulates the pii-DC phenotype. These findings define a developmental checkpoint, set by neuroendocrine maturation, that enables in situ DC activation and immune induction, thereby shaping age-dependent responses to allergens.
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Targeted dual biologic therapy for erythroderma of unknown etiology guided by high-parameter peripheral blood immunophenotyping
Type 2 immunity in allergic diseases
Data availability
All data to support the conclusions in this article can be found in the main text, extended data, supplementary information and source data. All genomic data generated in this study are publicly available at the Gene Expression Omnibus under accession numbers GSE273131, GSE299934 and GSE273161. The M. musculus reference genome (mm10/GRCm38) was used for sequencing alignment. We reanalysed the following publicly available dataset: GSE180542, GSE30999, public-accessible supplementary tables from Ewald et al.11, Dhingra et al.13, Renert-Yuval et al.19 and Del Duca et al.20. Source data are provided with this paper.
Code availability
The computational code used in this work can be found on GitHub (https://github.com/Naiklab/Pup-allergen-hypersensitivity-analysis-scripts).
References
Pierau, M., Arra, A. & Brunner-Weinzierl, M. C. Preventing atopic diseases during childhood — early exposure matters. Front. Immunol. 12, 617731 (2021).
Bakker, J. M., van Bel, F. & Heijnen, C. J. Neonatal glucocorticoids and the developing brain: short-term treatment with life-long consequences? Trends Neurosci. 24, 649–653 (2001).
Kaplan, H. S. et al. Sensory input, sex and function shape hypothalamic cell type development. Nature 647, 157–168 (2025).